Every day in my practice, I come across people who ask me about the difference between heat and ice therapy. Many people are not well-informed about the proper application of ice and heat therapy especially when it comes to the timing, duration, and frequency. First, I will go over the different phases of tissue repair following an injury. This is especially important because it will help in understanding why ice and heat are used in this context.
What is the body’s repair process after an injury?
Following an injury, the body goes through a systematic repair process. The repair process can be divided into 3 phases:
1) acute inflammation
2) post-acute repair / proliferation
3) remodeling.
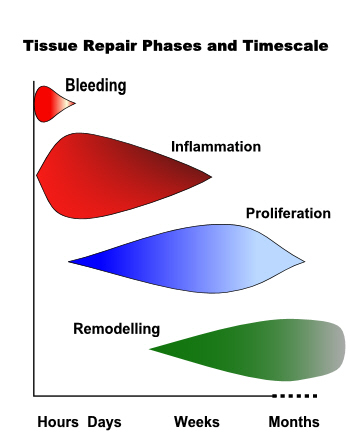
Phase 1: Acute Inflammation:
During the inflammatory phase, which usually lasts up to 72 hours, the main process involved is inflammation as the name suggests. Signs and symptoms of inflammation are pain, swelling, heat, redness, pressure, and loss of function and movement. Inflammation is part of the body’s innate and immediate response to a damaging stimulus/trauma/injury. The word inflammation usually has a negative connotation associated with it in therapeutic settings and it is often thought to be harmful for the body. However, it is an absolutely necessary first line of defence mechanism in our body that allows us to survive. Most importantly, inflammation allows the body to know the location and extent of an injury by activating the pain response. In addition, the dilation of blood vessels (vasodilation) allows blood cells and other substances to penetrate the damaged and surrounding tissues to start the repair/cleanup process. With that being said, too much or too long of an inflammatory process in the body can be damaging. Since inflammation is the body’s immediate response to an injury, the body never has adequate time to assess the extent of an injury, and therefore, the level of inflammation is usually much more exaggerated than what might be required. This is a cautionary measure by the body and it is the reason “inflammation” gets a negative connotation. Thus, during this inflammatory phase, the main goal of therapy is to reduce and control the level of inflammation.
This can be achieved by applying ice. Ice should be used along with the P.R.I.C.E. protocol. The price protocol is as follows:
- P = Protect
- R = Rest (To avoid further injuries)
- I = ICE (Ice or cold therapy reduces inflammation, pain, swelling, and must be used during the first 72h)
- C = Compression (Decreases swelling)
- E = Elevation (Increases the fluid drainage back to the heart)
Phase 2: Post-acute repair/proliferation:
The repair/proliferation phase usually lasts from 48 hours up to 4-6 weeks. During this phase, collagen, which is the main precursor to ligaments/tendons/connective tissues, gets deposited and proliferates into the different tissues. The deposition of collagen is done in a haphazard way and, therefore, the fibers are not properly oriented in the direction of maximal tensile strength. In addition, the quality of the collagen is inferior to the original and not as strong. The areas where collagen is deposited form a scab-like adhesion, that will become something called scar tissue if not treated properly. The clinical objective in this phase is to break adhesions, restore proper range of motion, decrease pain, and help reduce muscle spam and tightness.
Phase 3: Remodeling:
During the last phase, which lasts from 3-12 weeks or more, collagen is remodelled, strengthened, and oriented in the proper direction. The clinical objective during this phase is to restore full function, strength, flexibility, and range of motion. One way to increase the rate of repair in phase 2 and 3 is by increasing the blood flow to the injured area to allow metabolism to increase. This can be done by applying heat as it increases the body’s temperature and this, in turn, allows the body to increase blood flow and increase metabolism/repair. Heat also has pain-relieving characteristics and helps in relaxing muscles and tissues.
What are the effects of ice and heat?

Effects of heat:
- Decrease pain
- Increase metabolism
- Increase temperature
- Increase tissue repair
- Increase muscle and tissue relaxation
- Vasodilation
Effects of ice:
- Decrease pain
- Decrease inflammation
- Decrease swelling, edema
- Numbing effect
- Decrease Temperature
- Vasoconstriction
When do you apply ice/heat?
- Apply ice ONLY during phase 1 (follow the P.R.I.C.E. protocol); DO NOT apply heat
- Phase 2 & 3: heat and ice but mostly heat
- In these phases, ice therapy should only be used immediately after a treatment to decrease the local inflammation caused by deep tissue work. Heat should be used in between treatments.
How do you apply ice/heat? What protocols to follow for timing, frequency, and duration?
- General rule for both ICE & HEAT: 10-20 minutes on and 60 min off (tissues must return to normal temperature before 2nd application). Repeat the procedure 2-3 times per day.
- Wrap ice pack in a cold wet towel; wrap heat pack in a warm wet towel
- Never combine warming gel with a heat pack; never combine cooling gel/spray with ice; damaging to the tissues
- Never apply heat after an acute injury for the first 72 hours
- Never apply heat/ice before an exercise to mask the pain. Your body’s pain perception will decrease and you can potentially injure your body further
- Immediately after exercise, apply ice/cold therapy to decrease inflammation as exercise increases inflammation.